CORRECTIVE EXERCISE & THE BIOMECHANICS METHOD
The BioMechanics Method is the culmination of 30 plus years combined experience of Justin A. Price and Mary Bratcher working with sufferers of chronic pain.
The BioMechanics Method is the most effective Corrective Exercise program in the Fitness Industry. It helps people eliminate pain and dysfunctional movement patterns that contribute to this pain so they can begin or get back to an active lifestyle. By utilizing a thorough structural and movement assessment to pinpoint the SPECIFIC needs of each individual, practitioners of the BioMechanics Method are able to CREATE and DELIVER highly personalized exercise plans that correct issues more rapidly and successfully than other pain relief methods.
To be successful a Corrective Exercise Program must address imbalances and deviations in a logical format. Structures that have been damaged and stressed from misalignment must be reconditioned and realigned BEFORE any attempts at stretching or strengthening can made. This is similar to how metal is heated to enable it to be reshaped.
CORRECTIVE EXERCISE PROGRAM GOALS:
- Regenerate and release the fascia (film like tissue similar to shrink wrap that encases all muscles), muscles and tendons.
- Realign and increase blood flow and range of movement to the structures in question.
- Activate and Strengthen weak and or inactive muscles and retrain the nervous system to coordinate new movement patterns.
This is achieved through the implementation of THREE distinct phases:

1. Self-Myofascial Release
Self-Myofascial Release is used to rejuvenate and realign soft tissues which have been negatively affected by prolonged misalignment. Some people begin feeling relief from aches and pains right away with the implementation of this technique.

2. Stretching
Once irritated tissues have been rejuvenated and realigned, stretching helps to restore proper range of motion to the fascia, tendons and joints. This sets the stage for retraining proper movement in those parts of the body that have lost proper function through chronic misalignment.

3. Strengthening
This last stage of the program retrains the neuromuscular system (muscles and nerves that activate them) to coordinate to perform the new, proper movement patterns. You can get a chiropractic adjustment, but if the neuromuscular system has become accustomed to that dysfunctional alignment it will soon pull the bones back out of alignment. By retraining proper movement, we ensure that the musculoskeletal system remains in ideal alignment.
HOW POOR POSTURE AFFECTS YOUR HEALTH
Forward Head Posture

Poor posture isn’t just unattractive. It also has effects on your quality of life. For example, as can be seen from the image above just slight increases in forward positioning of your head can drastically increase the stress placed on your cervical spine. Some other effects of Forward Head Posture are as follows:
- Chronic Fatigue and Lack of Energy
- Decreases Lung Capacity By Up to 30%
- Dizziness, Vertigo & Poor Balance
- Impaired Vision & Hearing
- Early Degeneration of the Spine
- Neck & Jaw Pain
- Hormonal Imbalances
- Decreased Oxygen to the Brain
- Sinus Issues
- Pain in the Neck, Shoulders, Upper and/or Middle Back
- Headaches and Migraines
- Poor Sleep or Insomnia
- Arthritis
- Asthma
- Low Confidence
- Impaired Athletic Performance
- Appearing to be up to Two Inches Shorter Than You Actually Are
- Pinched Nerves (impedes signals to and from the brain from vital organs)
EXCESSIVE THORACIC KYPHOSIS (Hunch Back)
This condition can severely limit overhead pressing strength, decrease lung capacity as well as confidence and set one up for rotator cuff tears.
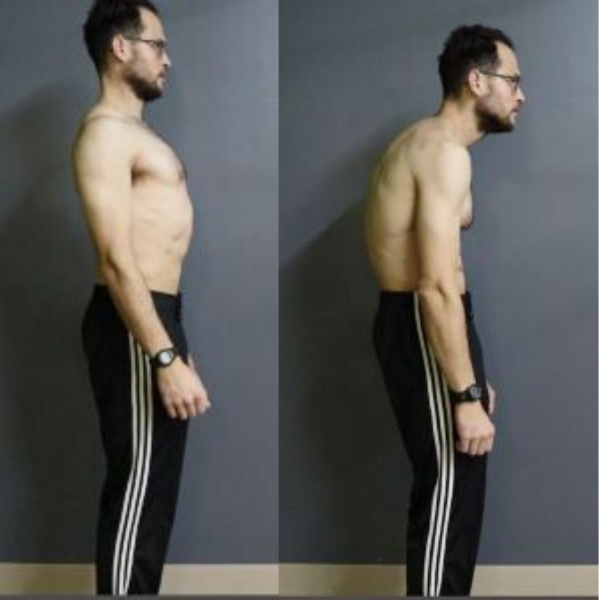
The Thoracic Spine has a normal Convex (outward curve). However, modern lifestyles as well as poor diet can make this curve excessive which in turn affects the alignment of the joints above and below the Thoracic Spine such as the neck and the hips.
When the shoulders slump forward the neck must arch back excessively to keep the eyes fixed on the horizon. As a result, the Flexors of the neck in the front become lax and weak, while the neck extensors become overly tight resulting in increased stress on the vertebra in this region, decreased blood flow and oxygen to the brain and inhibited function of the nerves in this area.
Additionally, when the shoulders are habitually stooped forward, the chest muscles become short and tight which will limit strength in exercises such as push-ups and the bench press.
Overhead pressing exercises and explosive movements such as Barbell Shoulder Presses and Barbell Snatches are also inhibited due to the inability to create a proper path for the bar when lifting overhead.
Most importantly, stooped shoulders cause misalignment at the Glenohumeral joint where the head of the upper arm bone and the bottom of the Acromion of the Scapula meet. If you picture a ball suspended in the middle of a ring by rubber bands this is similar to the structure of the shoulder joint. The shoulder joint allows for greater range of motion than any muscle in the body, but as such, sacrifices some stability. Care must be taken to keep the tension between the muscles acting on the head of the Humerus (upper arm bone) in balance. If balance is not maintained, the tendons of these muscles (usually the rotator cuff) can begin rubbing on the surrounding bone which, over time, will cause them to fray and eventually tear.
OTHER PROBLEMS ASSOCIATED WITH INCREASED THORACIC KYPHOSIS:
- Pain
- Limited Function
- Poor Health and Disease
- Increased Mental Stress
- Chronic fatigue and lack of energy
- Poor Sleep and Insomnia
- Arthritis
- Migraines
- Impaired Athletic Performance
- Loss of height by as much as 2”
- Decreased blood flow to the brain
- Early degeneration of the spine
- Hormonal disruption
- Looking 10lbs heavier than you actually are
- Dizziness, Vertigo and balance issues
- Decreased Range of Motion
- Decrease in Lung capacity by up to 30%
- Jaw pain and Sinus Issues
- Cagnie B, Dickx N, Peeters I, Tuytens J, Achten E,
Cambier D, Danneels L. (2008). The use of functional MRI to evaluate
cervical flexor activity during different cervical flexion exercises. J
Appl Physiol (1985). 2008 Jan;104(1):230-5. Epub 2007 Nov 8.
- Cailliet, R. and Leonard Gross, L. (1987). The
Rejuvenation Strategy: A Medically Approved Fitness Program to Reverse the
Effects of Aging. Doubleday and Company; 1st edition.
- Carney DR, Cuddy AJ, Yap AJ. (2010). Power posing:
brief nonverbal displays affect neuroendocrine levels and risk tolerance.
Psychol Sci. 2010 Oct;21(10):1363-8. doi: 10.1177/0956797610383437. Epub
2010 Sep 20.
- Dimitriadis Z, Kapreli E, Strimpakos N, Oldham J.
(2013). Respiratory weakness in patients with chronic neck pain. Man Ther.
2013 Jun;18(3):248-53. doi: 10.1016/j.math.2012.10.014. Epub 2012 Nov 28.
- Dusunceli Y, Ozturk C, Atamaz F, Hepguler S, Durmaz B.
Efficacy of neck stabilization exercises for neck pain: a randomized
controlled study. J Rehabil Med. 2009 Jul;41(8):626-31. doi:
10.2340/16501977-0392.
- Falla D, Jull G, Hodges P, Vicenzino B. (2006). An
endurance-strength training regime is effective in reducing myoelectric
manifestations of cervical flexor muscle fatigue in females with chronic
neck pain. Clin Neurophysiol. 2006 Apr;117(4):828-37. Epub 2006 Feb 21.
- Falla D, O’Leary S, Farina D, Jull G. (2012). The
change in deep cervical flexor activity after training is associated with
the degree of pain reduction in patients with chronic neck pain. Clin J
Pain. 2012 Sep;28(7):628-34. doi: 10.1097/AJP.0b013e31823e9378.
- Falla D, O’Leary S, Fagan A, Jull G. (2007).
Recruitment of the deep cervical flexor muscles during a
postural-correction exercise performed in sitting. Man Ther. 2007
May;12(2):139-43. Epub 2006 Aug 8.
- Fernández-de-las-Peñas C, Alonso-Blanco C, Cuadrado ML,
Gerwin RD, Pareja JA. (2006). Trigger points in the suboccipital muscles
and forward head posture in tension-type headache. Headache. 2006
Mar;46(3):454-60.
- Fernández-de-Las-Peñas C, Cuadrado ML, Pareja JA.
(2007). Myofascial trigger points, neck mobility, and forward head posture
in episodic tension-type headache. Headache. 2007 May;47(5):662-72.
- Griegel-Morris, P., Larson, K., Mueller-Klaus, K.,
Oatis, C.A. (1992) Incidence of Common Postural Abnormalities in the
Cervical, Shoulder, and Thoracic Regions and their Association with Pain
in Two Age Groups of Healthy Subjects. Physical Therapy. 72 (6), 425–431.
- Gupta BD, Aggarwal S, Gupta B, Gupta M, Gupta N.
(2013). Effect of Deep Cervical Flexor Training vs. Conventional Isometric
Training on Forward Head Posture, Pain, Neck Disability Index In Dentists
Suffering from Chronic Neck Pain. J Clin Diagn Res. 2013 Oct;7(10):2261-4.
doi: 10.7860/JCDR/2013/6072.3487. Epub 2013 Oct 5.
- Janda, V. (1988). Muscles and cervicogenic pain
syndromes. Physical therapy of the cervical and thoracic spine. Churchill
Livingstone.
- Kang DY. (2015). Deep cervical flexor training with a
pressure biofeedback unit is an effective method for maintaining neck
mobility and muscular endurance in college students with forward head
posture. J Phys Ther Sci. 2015 Oct;27(10):3207-10. doi:
10.1589/jpts.27.3207. Epub 2015 Oct 30.
- Kang JH, Park RY, Lee SJ, Kim JY, Yoon SR, Jung KI.
(2012). The effect of the forward head posture on postural balance in long
time computer based worker. Ann Rehabil Med. 2012 Feb;36(1):98-104. doi:
10.5535/arm.2012.36.1.98. Epub 2012 Feb 29.
- Kapreli E, Vourazanis E, Billis E, Oldham JA,
Strimpakos N. (2009). Respiratory dysfunction in chronic neck pain
patients. A pilot study. Cephalalgia. 2009 Jul;29(7):701-10. doi:
10.1111/j.1468-2982.2008.01787.x. Epub 2009 Feb 2.
- Kapandji, I. A. (2008). The Physiology of the Joints.
Churchill Livingstone; 6 edition.
- Lee MH1, Park SJ, Kim JS. (2013). Effects of neck
exercise on high-school students’ neck-shoulder posture. J Phys Ther Sci.
2013 May;25(5):571-4. doi: 10.1589/jpts.25.571. Epub 2013 Jun 29.
- Morningstar M. (2002). Cervical curve restoration and
forward head posture reduction for the treatment of mechanical thoracic
pain using the pettibon corrective and rehabilitative procedures. J
Chiropr Med. 2002 Summer;1(3):113-5. doi: 10.1016/S0899-3467(07)60013-5.
- Ozbek MM1, Miyamoto K, Lowe AA, Fleetham JA. 1998).
Natural head posture, upper airway morphology and obstructive sleep apnoea
severity in adults. Eur J Orthod. 1998 Apr;20(2):133-43.
- Park Y, Bae Y. (2014). Comparison of postures according
to sitting time with the leg crossed. J Phys Ther Sci. 2014
Nov;26(11):1749-52. doi: 10.1589/jpts.26.1749. Epub 2014 Nov 13.
- Erik Peper and I-Mei Lin (2012) Increase or Decrease
Depression: How Body Postures Influence Your Energy Level. Biofeedback:
Fall 2012, Vol. 40, No. 3, pp. 125-130.
- Silva AG, Punt TD, Sharples P, Vilas-Boas JP, Johnson
MI. (2009). Head posture and neck pain of chronic nontraumatic origin: a
comparison between patients and pain-free persons. Arch Phys Med Rehabil.
2009 Apr;90(4):669-74. doi: 10.1016/j.apmr.2008.10.018.
- Sato H, Ohashi J, Iwanaga K, Yoshitake R, Shimada K.
(1984). Endurance time and fatigue in static contractions. J Hum Ergol
(Tokyo). 1984 Dec;13(2):147-54.
- Sjøgaard G, Savard G, Juel C. (1988). Muscle blood flow
during isometric activity and its relation to muscle fatigue. Eur J Appl
Physiol Occup Physiol. 1988;57(3):327-35.
- Wilson VE, Peper E. (2004). The effects of upright and
slumped postures on the recall of positive and negative thoughts. Appl
Psychophysiol Biofeedback. 2004 Sep;29(3):189-95.
- Yoo WG. (2013). Effect of thoracic stretching, thoracic
extension exercise and exercises for cervical and scapular posture on
thoracic kyphosis angle and upper thoracic pain. J Phys Ther Sci. 2013
Nov;25(11):1509-10. doi: 10.1589/jpts.25.1509. Epub 2013 Dec 11.

